Evaluation of biocompatibility, osteointegration and biomechanical properties of the new Calcemex® cement: An in vivo study

All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Accepted: 11 January 2022
Authors
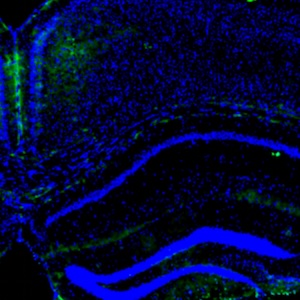
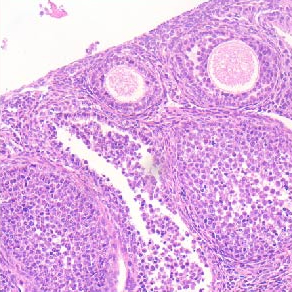
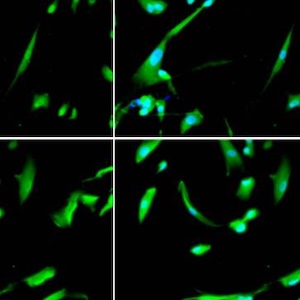
The mixture of polymethylmethacrylate (PMMA) and β-tricalciumphospate (β-TCP) is the most widely used bone graft. Common features of bone cement are the biocompatibility, bioactivity, mechanical stability and ability to fuse with the host's bone tissue. However, there are still few studies that have evaluated these characteristics in vivo. Our study aims to acquire these parameters, using an animal model with functional characteristics similar to those of humans. The analyzed cement is Calcemex®, evaluated both in compact and fluid formulation. The chosen animal models were 5 pigs, treated with femoral and tibial implants of Calcemex® samples. After one year, the pigs were sacrificed and the specimens explanted for morphological, histological, ultrastructural and mechanical evaluations. For both formulations, the investigation highlighted the absence of foreign body reactions in the host, the histological integration with the surrounding tissues and the preservation of mechanical compression resistance.
How to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.