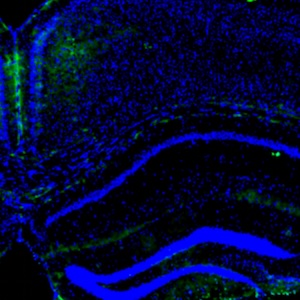
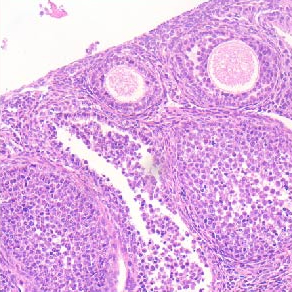
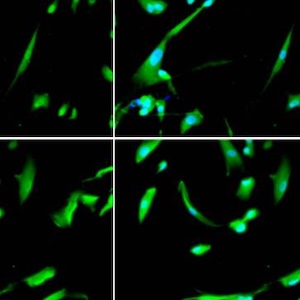
Swertianolin ameliorates immune dysfunction in sepsis via blocking the immunosuppressive function of myeloid-derived suppressor cells
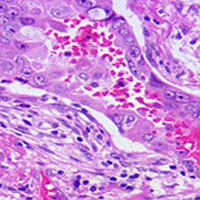
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Accepted: 26 July 2021
Authors
In this study, we studied the long-term proliferation trajectory of myeloid-derived suppressor cells (MDSCs) in murine sepsis model and investigated whether swertianolin could modulate the immunosuppressive function of MDSCs. A murine sepsis model was established by cecal ligation and perforation (CLP), according to the Minimum Quality Threshold in Pre-Clinical Sepsis Studies (MQTiPSS) guidelines. The bone marrow and spleen of the mice were collected at 24 h, 72 h, 7 and 15 d after sepsis induction. The proportions of monocytic-MDSCs (M-MDSCs; CD11b+LY6G-LY6Chi) and granulocytic-MDSCs (G-MDSC, CD11b+ Ly6G+ Ly6Clow) were analyzed by flow cytometry. Then, we have investigated whether swertianolin could modulate the immunosuppressive function of MDSCs in in vitro experiments. G-MDSCs and M-MDSCs increased acutely after sepsis with high levels sustained over a long period of time. G-MDSCs were the main subtype identified in the murine model of sepsis with polymicrobial peritonitis. Furthermore, it was found that swertianolin reduced significantly interleukin-10 (IL-10), nitric oxide (NO), reactive oxygen species (ROS), and arginase production in MDSCs, while reducing MDSC proliferation and promoting MDSC differentiation into dendritic cells. Swertianolin also improved T-cell activity by blocking the immunosuppressive effect of MDSCs. Both subsets of MDSCs significantly increased in the bone marrow and spleen of the mice with sepsis, with G-MDSCs being the main subtype identified. Swertianolin effectively regulated the functions of MDSCs and reduced immune suppression.
Department of Medical Intensive Care Unit, General Hospital of Southern Theater Command of PLA, Guangzhou;
Department of Critical Care Medicine, the Second Affiliated Hospital of Kunming Medical University, Kunming, China
Department of Medical Intensive Care Unit, General Hospital of Southern Theater Command of PLA, Guangzhou, China
How to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.