Mast cells in meningiomas
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Accepted: 19 March 2024
Authors
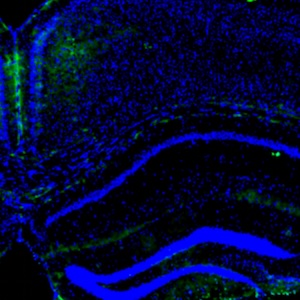
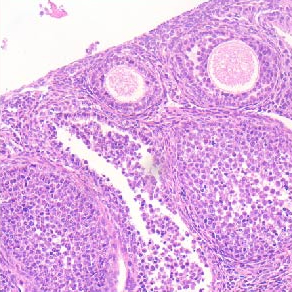
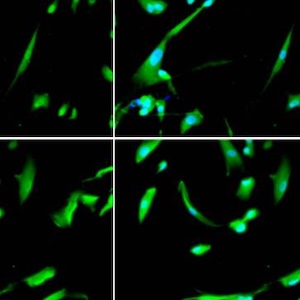
Meningioma represents the most frequent tumor of the central nervous system (CNS). Correlations between the presence of mast cells (MCs) and grade or other histological features of meningioma are still debated. Our study aimed to better understand the relationship between mast cells and meningiomas and to compare our results based on specific histological subtypes and novel 2021 CNS WHO grading system. We observed some differences as regards the number of MCs and meningioma grade. In low-grade (grade 1) meningiomas, MCs were observed in 7/22 cases, while they were consistently present in all eight high-grade cases (grade 2 and grade 3). Among the grade 1 meningiomas, we observed two “low-positive”, two “intermediate-positive”, and three “high-positive” cases. Among the group of high-grade meningiomas, the six cases grade 2 were considered as “low-positive”, while the two grade 3 cases showed a higher number of MCs and were included in the “intermediate-positive” group. Even though with no statistical significance, due to the low number of cases, our results seem to confirm a sort of relationship between meningioma grading and the number of MCs, as demonstrated by the higher percentage of high-grade meningiomas showing MCs infiltrates, compared to low-grade meningiomas.
Ethics Approval
this study was approved by the Institutional Review Board at the Bari Policlinico Hospital, University of Bari “Aldo Moro”Supporting Agencies
European Union Seventh Framework ProgramHow to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.