Effects of chronic exposure to bisphenol A in adult female mice on social behavior, vasopressin system, and estrogen membrane receptor (GPER1)

All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Accepted: 20 October 2021
Authors
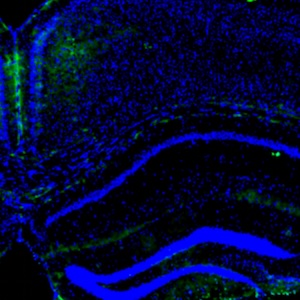
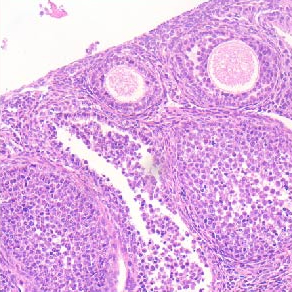
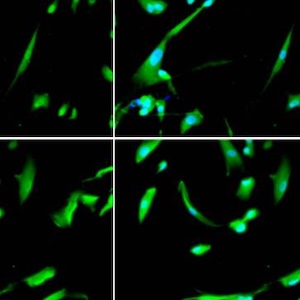
Bisphenol A (BPA), an organic synthetic compound found in some plastics and epoxy resins, is classified as an endocrine disrupting chemical. Exposure to BPA is especially dangerous if it occurs during specific “critical periods” of life, when organisms are more sensitive to hormonal changes (i.e., intrauterine, perinatal, juvenile or puberty periods). In this study, we focused on the effects of chronic exposure to BPA in adult female mice starting during pregnancy. Three months old C57BL/6J females were orally exposed to BPA or to vehicle (corn oil). The treatment (4 µg/kg body weight/day) started the day 0 of pregnancy and continued throughout pregnancy, lactation, and lasted for a total of 20 weeks. BPA-treated dams did not show differences in body weight or food intake, but they showed an altered estrous cycle compared to the controls. In order to evidence alterations in social and sociosexual behaviors, we performed the Three-Chamber test for sociability, and analyzed two hypothalamic circuits (well-known targets of endocrine disruption) particularly involved in the control of social behavior: the vasopressin and the oxytocin systems. The test revealed some alterations in the displaying of social behavior: BPA-treated dams have higher locomotor activity compared to the control dams, probably a signal of high level of anxiety. In addition, BPA-treated dams spent more time interacting with no-tester females than with no-tester males. In brain sections, we observed a decrease of vasopressin immunoreactivity (only in the paraventricular and suprachiasmatic nuclei) of BPA-treated females, while we did not find any alteration of the oxytocin system. In parallel, we have also observed, in the same hypothalamic nuclei, a significant reduction of the membrane estrogen receptor GPER1 expression.
How to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.