Histopathological and immunofluorescent characterization of post-sepsis immune dysregulation in a clinically relevant mouse model

All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Authors
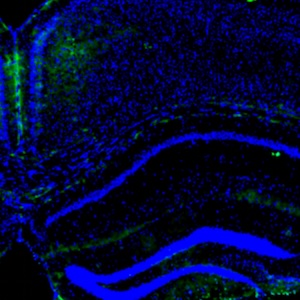
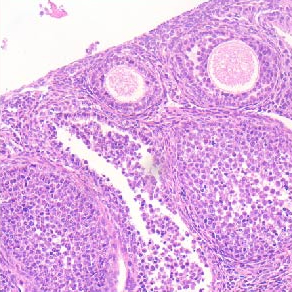
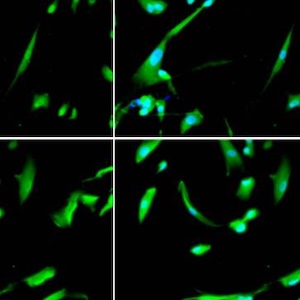
Sepsis remains a major cause of morbidity and mortality worldwide, yet its prolonged pathophysiological consequences are poorly understood. Here, we employed a murine cecal ligation and puncture (CLP) model to investigate the prolonged impact of sepsis on survival, systemic inflammation, and organ pathology. Adult male C57BL/6 mice underwent CLP or sham surgery and were monitored for 28 days. Survival was recorded daily, while serial assessments of hematology, serum biochemistry, bacterial load, and cytokine levels were performed. Tissue immunofluorescence was used to characterize myeloid-derived suppressor cells (MDSCs), which are potent immunosuppressive cells that inhibit both adaptive and innate immune responses in sepsis, contributing to sepsis-induced immunosuppression. Histopathological analyses were conducted to evaluate structural changes in major organs. CLP mice displayed markedly reduced long-term survival compared with sham controls. Hematological profiling revealed persistent leukocytosis and an inflammatory response, while serum analyses showed sustained elevations in in bilirubin, creatinine, and blood urea nitrogen, reflecting hepatic and renal injury. Bacterial cultures confirmed systemic microbial persistence, and cytokine measurements indicated ongoing inflammatory activity. Tissue immunofluorescence demonstrated the infiltration of MDSCs across multiple organs, consistent with post-sepsis immunosuppression. Histopathological examination revealed widespread, chronic injury in the lungs, liver, kidneys, and spleen, including inflammatory infiltration, tissue degeneration, and architectural disruption. In conclusion, sepsis induces not only acute systemic inflammation but also enduring immune dysregulation and progressive organ damage. These findings highlight the CLP model as a robust platform for studying post-sepsis sequelae and underscore the need for therapeutic strategies that target long-term organ protection and immune restoration.
Ethics Approval
this study was approved by the Animal Experiment Ethics Review Committee of Kunming Medical University (Approval number: Kmmu20230225)CRediT authorship contribution
Zongfang Ren, Haoran Tang, study conception and design, funding support; Lingling Wang, methodology; Ning Tang, data curation; Haoran Tang, Chen Liao, data analysis and interpretation; Zongfang Ren, supervision. All authors, writing – original draft, review and editing. All authors read and approved the final manuscript.
Supporting Agencies
Basic Research Program of the Science and Technology Department of Yunnan Province, Yunnan Science and Technology Department’s plan for cultivating science and technology talents and establishing platformsData Availability Statement
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request
How to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.